Overview
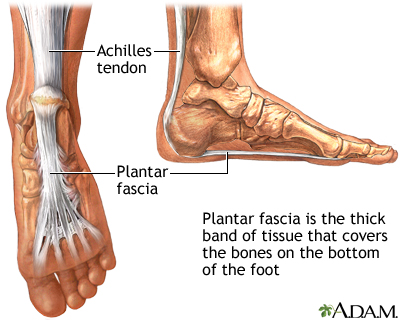
Most flat feet are not painful, particularly those flat feet seen in children. In the adult acquired flatfoot, pain occurs because soft tissues (tendons and ligaments) have been torn. The deformity progresses or worsens because once the vital ligaments and posterior tibial tendon are lost, nothing can take their place to hold up the arch of the foot. The painful, progressive adult acquired flatfoot affects women four times as frequently as men. It occurs in middle to older age people with a mean age of 60 years. Most people who develop the condition already have flat feet. A change occurs in one foot where the arch begins to flatten more than before, with pain and swelling developing on the inside of the ankle. Why this event occurs in some people (female more than male) and only in one foot remains poorly understood. Contributing factors increasing the risk of adult acquired flatfoot are diabetes, hypertension, and obesity.
Causes
Plantar Fasciitis is commonly the cause of most arch pain. The bands of fibrous tissue in the arches of the feet become inflamed. Plantar Fasciitis is associated with early morning arch pain, from the plantar fascia tightening and contracting during the night when there is no strain on the bands. Arch pain occurs when there are extended periods of standing or walking, resulting in prolonged tension on the plantar fascia which in turn causes inflammation and irritation. While plantar fasciitis normally affects middle aged men and women, younger athletes are affected by arch pain because of the repetitive movement of certain sports, which causes damage to the fibrous tissue.
Symptoms
Bones and ligaments work together to form joints, and bones are joined together by ligaments. Strains occur in ligaments. In the arch, there are ligaments that are located at the ends of each bone. These ligaments connect the bones to other bones on both ends and on the sides. Point tenderness and looseness of a joint are indicators of a sprain. Fractures are indicated by point tenderness that may be severe over the area of bone that is affected. There may be a distinguishable lump or gap at the site of the fracture. A rotated toe or forefoot may also be a sign of a fracture.
Diagnosis
The doctor will examine your feet for foot flexibility and range of motion and feel for any tenderness or bony abnormalities. Depending on the results of this physical examination, foot X-rays may be recommended. X-rays are always performed in a young child with rigid flatfeet and in an adult with acquired flatfeet due to trauma.
Non Surgical Treatment
In mild cases of flatfoot the first line of treatment is often custom orthotics. In patients with a flexible deformity, supporting the arch with a custom arch support will take the strain off the joints and muscles, bringing the heel into a corrected position. Wider shoe gear may be prescribed to accommodate foot pain and motion and stretching exercises to decrease stiffness and stress on the foot. In cases of severe collapse, especially if the patient is not a good surgical candidate or has a mild tear, a brace may be made to accommodate the foot and ankle, thus supporting the arch and ankle.

Surgical Treatment
In rare cases, surgery may be needed if a child has flat feet caused by a problem they're born with (a congenital abnormality). The foot may need to be straightened or the bones may need to be separated if they're fused together. Painkillers and insoles are the first treatment options for flat feet that are caused by a joint problem, such as arthritis or a torn tendon. However, surgery may be recommended if the injury or condition is severely affecting your feet. Where flat feet are caused by a condition that affects the nervous system, special shoes, insoles, or supportive foot or leg braces may be needed. Again, in severe cases, an operation may be needed to straighten the feet.
Prevention
Because most cases of flatfeet are inherited, the condition is usually impossible to prevent. Even when children with flexible flatfeet are treated with arch supports and corrective shoes, there is little evidence that these devices prevent the condition from lasting into adulthood.
Stretching Exercises
Plantar Fasciitis stretches can be incorporated into a comprehensive treatment regime which may involve: ice, heel wedge support, taping, massage, muscle strengthening, orthotic inserts for shoes, topical anti inflammatory gel or oral medication and/or corticosteroid injections. If you suspect you may have Plantar Fasciitis seek accurate diagnosis and treatment from a health professional to ensure a correct diagnosis and reduce the likelihood of developing chronic foot pain. Treatment interventions may be provided by your Physical Therapist, Podiatrist and/or doctor.
Most flat feet are not painful, particularly those flat feet seen in children. In the adult acquired flatfoot, pain occurs because soft tissues (tendons and ligaments) have been torn. The deformity progresses or worsens because once the vital ligaments and posterior tibial tendon are lost, nothing can take their place to hold up the arch of the foot. The painful, progressive adult acquired flatfoot affects women four times as frequently as men. It occurs in middle to older age people with a mean age of 60 years. Most people who develop the condition already have flat feet. A change occurs in one foot where the arch begins to flatten more than before, with pain and swelling developing on the inside of the ankle. Why this event occurs in some people (female more than male) and only in one foot remains poorly understood. Contributing factors increasing the risk of adult acquired flatfoot are diabetes, hypertension, and obesity.

Causes
Plantar Fasciitis is commonly the cause of most arch pain. The bands of fibrous tissue in the arches of the feet become inflamed. Plantar Fasciitis is associated with early morning arch pain, from the plantar fascia tightening and contracting during the night when there is no strain on the bands. Arch pain occurs when there are extended periods of standing or walking, resulting in prolonged tension on the plantar fascia which in turn causes inflammation and irritation. While plantar fasciitis normally affects middle aged men and women, younger athletes are affected by arch pain because of the repetitive movement of certain sports, which causes damage to the fibrous tissue.
Symptoms
Bones and ligaments work together to form joints, and bones are joined together by ligaments. Strains occur in ligaments. In the arch, there are ligaments that are located at the ends of each bone. These ligaments connect the bones to other bones on both ends and on the sides. Point tenderness and looseness of a joint are indicators of a sprain. Fractures are indicated by point tenderness that may be severe over the area of bone that is affected. There may be a distinguishable lump or gap at the site of the fracture. A rotated toe or forefoot may also be a sign of a fracture.
Diagnosis
The doctor will examine your feet for foot flexibility and range of motion and feel for any tenderness or bony abnormalities. Depending on the results of this physical examination, foot X-rays may be recommended. X-rays are always performed in a young child with rigid flatfeet and in an adult with acquired flatfeet due to trauma.
Non Surgical Treatment
In mild cases of flatfoot the first line of treatment is often custom orthotics. In patients with a flexible deformity, supporting the arch with a custom arch support will take the strain off the joints and muscles, bringing the heel into a corrected position. Wider shoe gear may be prescribed to accommodate foot pain and motion and stretching exercises to decrease stiffness and stress on the foot. In cases of severe collapse, especially if the patient is not a good surgical candidate or has a mild tear, a brace may be made to accommodate the foot and ankle, thus supporting the arch and ankle.

Surgical Treatment
In rare cases, surgery may be needed if a child has flat feet caused by a problem they're born with (a congenital abnormality). The foot may need to be straightened or the bones may need to be separated if they're fused together. Painkillers and insoles are the first treatment options for flat feet that are caused by a joint problem, such as arthritis or a torn tendon. However, surgery may be recommended if the injury or condition is severely affecting your feet. Where flat feet are caused by a condition that affects the nervous system, special shoes, insoles, or supportive foot or leg braces may be needed. Again, in severe cases, an operation may be needed to straighten the feet.
Prevention
Because most cases of flatfeet are inherited, the condition is usually impossible to prevent. Even when children with flexible flatfeet are treated with arch supports and corrective shoes, there is little evidence that these devices prevent the condition from lasting into adulthood.
Stretching Exercises
Plantar Fasciitis stretches can be incorporated into a comprehensive treatment regime which may involve: ice, heel wedge support, taping, massage, muscle strengthening, orthotic inserts for shoes, topical anti inflammatory gel or oral medication and/or corticosteroid injections. If you suspect you may have Plantar Fasciitis seek accurate diagnosis and treatment from a health professional to ensure a correct diagnosis and reduce the likelihood of developing chronic foot pain. Treatment interventions may be provided by your Physical Therapist, Podiatrist and/or doctor.
 The Achilles tendon, or calcaneal tendon, is a large ropelike band of fibrous tissue in the back of the ankle that connects the powerful calf muscles to the heel bone (calcaneus). Sometimes called the heel cord, it is the largest tendon in the human body. When the calf muscles contract, the Achilles tendon is tightened, pulling the heel. This allows you to point your foot and stand on tiptoe. It is vital to such activities as walking, running, and jumping. A complete tear through the tendon, which usually occurs about 2 inches above the heel bone, is called an Achilles tendon rupture. Causes Factors that may increase your risk of Achilles tendon rupture include Age. The peak age for Achilles tendon rupture is 30 to 40. Your sex. Achilles tendon rupture is up to five times more likely to occur in men than in women. Playing recreational sports. Achilles tendon injuries occur more often in sports that involve running, jumping and sudden starts and stops - such as soccer, basketball and tennis. Steroid injections. Doctors sometimes inject steroids into an ankle joint to reduce pain and inflammation. However, this medication can weaken nearby tendons and has been associated with Achilles tendon ruptures. Certain antibiotics. Fluoroquinolone antibiotics, such as ciprofloxacin (Cipro) or levofloxacin (Levaquin), increase the risk of Achilles tendon rupture. Symptoms Whereas calf strains and tendonitis may cause tightness or pain in the leg, Achilles tendon ruptures are typically accompanied by a popping sensation and noise at the time of the injury. In fact, some patients joke that the popping sound was loud enough to make them think they?d been shot. Seeing a board-certified orthopedic surgeon is the best way to determine whether you have suffered an Achilles tendon tear. Diagnosis The diagnosis of an Achilles tendon rupture can be made easily by an orthopedic surgeon. The defect in the tendon is easy to see and to palpate. No x-ray, MRI or other tests are necessary. Non Surgical Treatment Once the Achilles tendon is partially damaged, one should exercise great care. The risk of rupture is high and if pain is associated with walking, one should consult with an orthopedic surgeon or a sports physician. A complete rupture of the Achilles tendon is never treated at home. It is important to understand that there are no minerals, nutrients, or herbs to treat Achilles tendon injury and any delay just worsens the recovery.
The Achilles tendon, or calcaneal tendon, is a large ropelike band of fibrous tissue in the back of the ankle that connects the powerful calf muscles to the heel bone (calcaneus). Sometimes called the heel cord, it is the largest tendon in the human body. When the calf muscles contract, the Achilles tendon is tightened, pulling the heel. This allows you to point your foot and stand on tiptoe. It is vital to such activities as walking, running, and jumping. A complete tear through the tendon, which usually occurs about 2 inches above the heel bone, is called an Achilles tendon rupture. Causes Factors that may increase your risk of Achilles tendon rupture include Age. The peak age for Achilles tendon rupture is 30 to 40. Your sex. Achilles tendon rupture is up to five times more likely to occur in men than in women. Playing recreational sports. Achilles tendon injuries occur more often in sports that involve running, jumping and sudden starts and stops - such as soccer, basketball and tennis. Steroid injections. Doctors sometimes inject steroids into an ankle joint to reduce pain and inflammation. However, this medication can weaken nearby tendons and has been associated with Achilles tendon ruptures. Certain antibiotics. Fluoroquinolone antibiotics, such as ciprofloxacin (Cipro) or levofloxacin (Levaquin), increase the risk of Achilles tendon rupture. Symptoms Whereas calf strains and tendonitis may cause tightness or pain in the leg, Achilles tendon ruptures are typically accompanied by a popping sensation and noise at the time of the injury. In fact, some patients joke that the popping sound was loud enough to make them think they?d been shot. Seeing a board-certified orthopedic surgeon is the best way to determine whether you have suffered an Achilles tendon tear. Diagnosis The diagnosis of an Achilles tendon rupture can be made easily by an orthopedic surgeon. The defect in the tendon is easy to see and to palpate. No x-ray, MRI or other tests are necessary. Non Surgical Treatment Once the Achilles tendon is partially damaged, one should exercise great care. The risk of rupture is high and if pain is associated with walking, one should consult with an orthopedic surgeon or a sports physician. A complete rupture of the Achilles tendon is never treated at home. It is important to understand that there are no minerals, nutrients, or herbs to treat Achilles tendon injury and any delay just worsens the recovery.  Surgical Treatment In general, Achilles tendon repair surgery has a much higher success rate and lower incidences of re-rupture than non-surgical methods of treatment. It is preferred by the nation?s leading athletes as the best course of action, allowing them to return to previous activity and performance levels at a much faster rate, with a lower chance or re-injury and less potential muscle loss.
Surgical Treatment In general, Achilles tendon repair surgery has a much higher success rate and lower incidences of re-rupture than non-surgical methods of treatment. It is preferred by the nation?s leading athletes as the best course of action, allowing them to return to previous activity and performance levels at a much faster rate, with a lower chance or re-injury and less potential muscle loss.






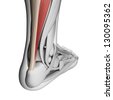 The Achilles tendon is a conjoined tendon composed of the gastrocnemius and soleus muscles with occasional contribution from the plantaris muscle, and it inserts on the calcaneal tuberosity. The plantaris muscle is absent in 6% to 8% of individuals. The Achilles tendon is approximately 15-cm long and is the largest and strongest tendon in the human body. The tendon spirals approximately 90 from its origin to its insertion and this twisting produces an area of stress approximately 2- to 5-cm proximal to its insertion. The tendon has no true synovial sheath; instead it is wrapped in a paratenon. The Achilles tendon experiences the highest loads of any tendon in the body, and bears tensile loads up to 10 times body weight during athletic activities. The tendon most commonly ruptures in a region 2- to 6-cm proximal to its insertion.
The Achilles tendon is a conjoined tendon composed of the gastrocnemius and soleus muscles with occasional contribution from the plantaris muscle, and it inserts on the calcaneal tuberosity. The plantaris muscle is absent in 6% to 8% of individuals. The Achilles tendon is approximately 15-cm long and is the largest and strongest tendon in the human body. The tendon spirals approximately 90 from its origin to its insertion and this twisting produces an area of stress approximately 2- to 5-cm proximal to its insertion. The tendon has no true synovial sheath; instead it is wrapped in a paratenon. The Achilles tendon experiences the highest loads of any tendon in the body, and bears tensile loads up to 10 times body weight during athletic activities. The tendon most commonly ruptures in a region 2- to 6-cm proximal to its insertion.
 RSS Feed
RSS Feed
